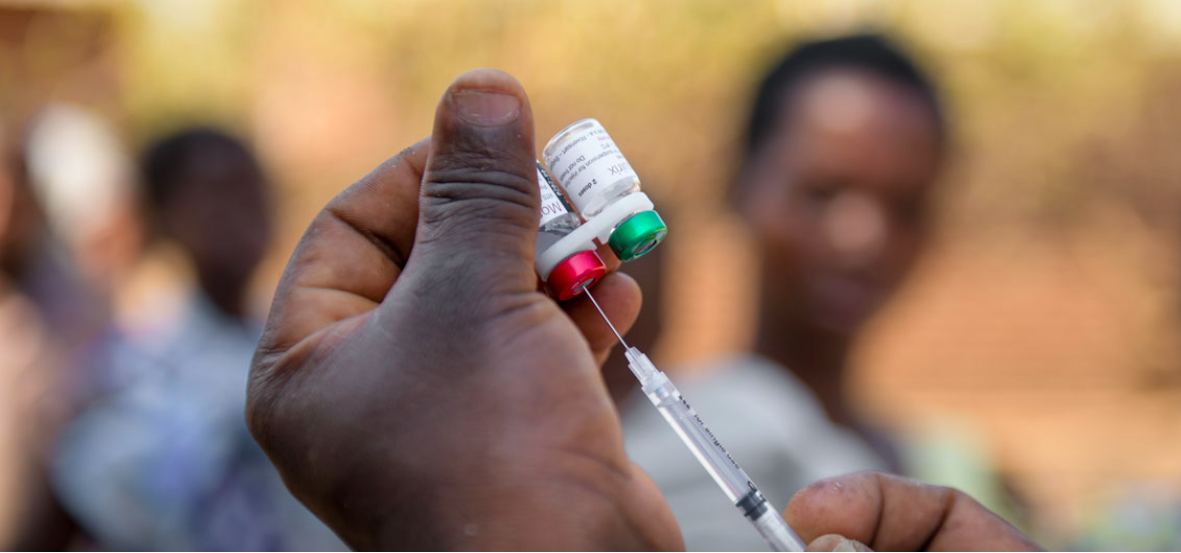
 A pilot in Kenya, Ghana and Malawi generated evidence that the introduction of the vaccine resulted in a 13 per cent reduction in all-cause mortality among children.
A pilot in Kenya, Ghana and Malawi generated evidence that the introduction of the vaccine resulted in a 13 per cent reduction in all-cause mortality among children.
Uganda has
become the latest country to introduce a malaria vaccine.
Uganda adopted the R21 vaccine, which has not been introduced in Kenya's routine immunisation.
Uganda rolled out the vaccination campaign in northern region, according to a statement from the financier, Gavi. This makes Uganda the 19th country in Africa to introduce a malaria vaccine into routine immunisation, and it is the largest malaria vaccine roll-out to date in terms of target districts and population.
Kenya introduced the RTS,S malaria vaccine in 2019.
Both the RTS,S/AS01 and R21/Matrix-M vaccines, are prequalified and recommended by the World Health Organization to prevent malaria in children.
The R21/Matrix-M malaria vaccine, administered in four doses at 6, 7, 8 and 18 months, will initially target 1.1 million children aged under two years in 105 high- and moderate-transmission districts across Uganda, with plans to expand nationwide, the statement said.
Apac District is reported to have the highest number of mosquito bites per person globally (over 1,500 bites per person annually).
Malaria is the leading cause of illness and death among young children in Uganda, responsible for up to 33 per cent of all outpatient visits, 22 per cent of hospital admissions and six per cent of deaths, according to 2023 data from WHO.
In 2023, Uganda was among the top five African countries with the highest malaria burden, alongside Nigeria, Democratic Republic of the Congo, Ethiopia and Mozambique.
The Minister of Health, Dr Jane Ruth Aceng Ocero, said: “The introduction of the vaccine marks a significant milestone in our fight against malaria. It is expected to prevent at least 800 cases of severe malaria among children every day and ease the financial burden on families.”
To date, Gavi has supported 19 African countries in integrating the malaria vaccine into routine immunisation programmes.
Gavi’s model relies on co-financing, meaning that countries contribute to the cost of their own vaccines, paying progressively more as their income rises to the point where they fully pay for their own programmes.
Future support for its global malaria programme is dependent
on Gavi securing sufficient funds for its next five-year strategic period
starting in 2026.
Any shortfall in funding will result in programmes being cut back, leading to preventable deaths and a greater threat to global health security, Gavi said.
Commenting on the roll-out, Dr Sania Nishtar, CEO of Gavi, said: “The malaria vaccine, proven safe and effective, saves lives and prevents hospitalisations. However, without sustained financial support, these life-saving efforts could falter, leaving millions of children vulnerable and undermining the progress made so far. Continued funding is crucial to sustain and expand these efforts, ensuring that more children are protected, and more countries benefit from this vital tool.”
WHO coordinated the pilot evaluation of the first malaria vaccine, RTS,S/AS01, which was co-funded by Gavi and other partners.
Through a multiyear programme in Kenya, Ghana and Malawi, the pilot generated evidence that the introduction of the vaccine resulted in a 13 per cent reduction in all-cause mortality among children.
This led to WHO’s recommendation and prequalification of the two malaria vaccines available today. WHO continues to support countries by providing guidance, sharing experiences and offering technical assistance to ensure successful implementation.











